To view our Privacy Policy please click below


Supporting the North West Centre for Heart & Lung Transplantation
Lyn Rose
MY HEART TRANSPLANTATION JOURNEY – BY LYN ROSE
Having read the other patient stories on this web site and others on line I felt encouraged to write mine. I didn’t know what to include and I’m not a medical person, so this is written in my own words with my own understanding, with some of the medical facts double checked in case my memory didn’t serve me too well. If you are reading this and you are on the transplant list, or considering organ donation, I hope you will be very much encouraged about the difference a new heart can make to someone’s life.
Firstly, I have nothing but praise and appreciation for all the expertise, care and compassion from all the medics who have treated me pre, during and post transplant, so don’t believe all the bad reports about our NHS. The people who have been involved in my care over the years are such a credit to their profession and deserve all the support and respect due to them.
I was diagnosed with Hypertrophic Cardiomyopathy in 1996, aged 33. I was going to the gym regularly but was getting breathless after only 10 minutes on the exercise bike or treadmill and didn’t progress. I was very lean and strong with no excess weight and just didn’t understand why I wasn’t doing as well as I’d expected.
My maternal Grandmother had died soon after my mother was born. She was only 36 and had severe heart failure. My mother had died in 1990 at 54 years of age of heart failure and her death certificate said ‘Cardiomyopathy’. I had heard on the TV of a lady with similar symptoms that I was experiencing and she was suffering from an hereditary condition. I decided to see my GP who referred me to my local hospital for tests. The Cardiologist confirmed that my heart was enlarged and was probably due to the same genetic heart disease my mother had died of.
I was not having palpitations or light-headedness so it was decided that I would be checked every year. I stopped sprinting for the train and pushing myself at the gym and just stuck to cardio vascular exercises. It was a while before it struck me that when I was a lot younger, the symptoms were manifesting. I had a very active, sporty childhood, but I could never do a cross country run without feeling like someone was crushing my chest. I could run a fast 100 metre race for the school but struggled with 400 metre jog. Looking back it started to make sense.
I carried on a very busy life, working, bringing up two active children and very much involved in our local church ministries. My heart would occasionally go very fast and bounce around and then settle after a few minutes into normal rhythm. This wasn’t regularly, so I wasn’t really too concerned.
On 9th June 2008 I enjoyed a long walk with a friend. It was a hot day and I probably became a bit too dehydrated. I felt ill when I returned home and just drank a lot. The next day as soon as I got out of bed my heart went mad. Racing and banging around very uncomfortably in my chest.
I had various tests and they said my heart was in AF (Atrial Fibrillation). Six weeks later, after a course of anticoagulants I had a successful cardioversion, this is when the heart is stopped and restarted back into regular rhythm.
I took a while to recover my strength back and return to work. I was a lot slower at doing everything but still had quite an active life. I used to love to sing and had vocal training but after this episode I found it very exhausting to sing properly.
I continued to do a lot of walking, being careful not to get too tired and was very encouraged with increased stamina.
On 1st June 2012 I got out of bed in the morning and my heart went into AF again. It was the weekend of the Queen’s Golden Jubilee and I really didn’t want to go into hospital during a four day bank holiday. By the Monday my rhythm hadn’t settled so I reluctantly went in to my local A & E. I was in for two weeks and the tests showed that a cardioversion would probably not be successful. Dr. Jay Wright, my Cardiologist at the Liverpool Heart and Chest Hospital put me on a drug called Amiodarone for six weeks with a view to trying another cardioversion. This was successful but unfortunately in November 2012 my heart went into AF again. I was admitted to the Critical Care Unit in LHCH. I couldn’t sit up or pick up a cup of tea without my heart racing rapidly out of rhythm. When I slept my heart rate was only beating about 30bpm and they kept waking me up! I was kept in CCU for about three days and then transferred to a ward.
I was fitted with a bi-ventricular implantable cardioverter defibrillator (ICD). Dr.Stephen Pettit carried out the procedure. This made a noticeable difference to my mobility as this and medication stabilised my heart, but I noticed that I had deteriorated quite substantially following this latest period of being in AF. My heart was still out of rhythm but much more controlled. I attended Cardiac rehab to gain muscle strength and started doing more walking with my dog and family.
Dr. Pettit referred me to Dr. Steven Shaw at Wythenshawe for heart transplant assessment and I went through the usual five day testing in August 2013. I was put on the active transplant list in October 2013 and got on with my life. I was still shopping, doing housework and gardening, socialising and working from home right up to the day before the transplant. Mobile activity was slow going and I used to have to stop three times between the kitchen and the car on the drive just to get my breath, but it didn’t stop me going out. I was given a Blue Badge for parking which helped.
My assessment for a transplant confirmed that due to my blood group which is B+ and various antibodies the ‘chances’ of a donor heart being a suitable match was 15%. I don’t live by chance. I have a very strong Christian faith and I live by faith. I believed that if I was meant to have a heart transplant then the perfect donor heart would be gifted to me. I wasn’t sitting around waiting for the phone to ring; I was just very slowly getting on with life but experiencing my mobility getting slower and slower.
My angiogram in November 2013 showed that the pressures in my heart weren’t very good at all. The left side of my heart was very enlarged and very little oxygenated blood was being pumped around my body. Dr. Shaw said that there were people who had better results in the Intensive Care unit awaiting an emergency transplant. He said the rest of my body was compensating really well and I looked well.
On Friday 4th April 2014 I was sitting having a my second cup of Earl Grey, planning my day ahead, when I received a call from Laura, one of the Transplant Coordinators at Wythenshawe. She said a donor heart had become available that was very suitable for me. I was so shocked. When I put the phone down I could hardly get the words out to tell my husband what Laura had said. I became quite emotional at first then just went into auto pilot mode and quickly got myself and my bag ready. I had a little wobble when I hugged my two children as I said goodbye. For a split second I thought ‘What if I don’t see them again’. But as soon as that thought came, I spoke out “See you both tomorrow”. I said to my husband. “There will be no negative ‘what ifs’. If this is going ahead, then it’s going ahead and everything will be fine”. We both had a real peace about it on the way, apart from when the traffic came to a standstill on the M6 at the Thelwall Viaduct and we just sat there for what seemed like ages. I phoned the Transplant Centre and explained but was assured by one of the Coordinators that a short delay wouldn’t be of concern to them. We arrived at the Jim Quick ward about midday and the time flew as I went through all the preparation for the operation. Lots of paper work, questions to be asked and answered and people to meet who were involved in the operation.
My husband Adrian said “I really think everything will be fine and they’ll all be amazed at your recovery”. I was still very calm about everything. At the back of my mind I thought it may be a false alarm and we’d be home for teatime with a story to tell. This may sound like denial, it wasn’t, I was just very much at peace about whether or not I was going to receive a new heart, or not that day.
I was taken into the anaesthetic room at about 4.30. Adrian was allowed with me, which was nice. As the Anaesthetist was putting a line in Laura came in to the room with a big smile on her face and said “Your transplant is going ahead and they’re ready for you”. Adrian kissed me goodbye and the last thing I heard was Laura saying “see you after your operation”.
The next thing I knew a lovely nurse was waking me up. It was the next morning. I could hear horse racing in the distance and asked her if it was the Grand National. Another patient in the Critical Care Unit must have been watching the racing from Aintree. I was really thirsty and wanted a cup of tea. I had water to begin with. A little later I sat up and was mercifully given a lovely cup of Earl Grey (I always take my own tea bags with me). One of the doctors said I’d asked him for a cup of tea when I was coming round earlier on. I remembered asking him and taking his hand and writing a letter ‘T’ on his palm. At the time I thought I’d dreamt this. Whilst coming around from the anaesthetic I was unsure what I’d dreamt and what had actually taken place. I probably had the same conversations with my nurse over and over.
That afternoon my husband and two (adult) children came in to see me. I was wired up to lots of machines, but their faces didn’t show any shock at all the leads and wires. They’d seen me in CCU in Liverpool . My daughter was concerned about an octopus looking lead which was coming out of my neck and stitched to my cheek to support it. I was sitting up chatting to them and drinking more tea, so they were pleased and relieved.
My nurse and a physiotherapist got me out of bed that afternoon and I just walked on the spot for a about a minute. I felt great. My balance was good and I was able to get back on the bed without much help. They were really pleased and encouraging. My family came back again for the evening visit and I was a lot more awake. I was hungry but advised not to eat anything at that stage.
The next morning I had a bowl of bran flakes and more tea and fruit juice. The nurse took the feeding tube from down my throat as I hadn’t needed it. I had a vegetable roast for lunch but my husband had to cut it up for me as I felt a bit shaky using the knife and fork. That afternoon I had a walk up the ward and back. I was already noticing that I wasn’t as breathless as I’d been before the transplant. Mr. Ali my surgeon came to visit me and assured me that I had been given a good strong heart. He was very pleased with my progress, as were all the other doctors who kept visiting me.
On the Monday, day 3 Dr. Steve Shaw was back on duty and he came to see me with a huge smile on his face. He looked closer at the machinery around me and said “I can’t believe how well you are doing, this is amazing”. Not to detract from the wonderful medical care and expertise of the medics, I believe that the vast amount of prayer from around the world for me played a big part in my amazing recovery. That afternoon I walked down the ward, out of the door and did a circular walk along a corridor and round in another door to the ward and back to my bed. I sat in a lovely comfortable chair until bedtime reading and watching some tv.
It was on this day, sitting in the Critical Care Unit looking around at all the beds and hundreds of wires and machines that it really struck me that I’d had a heart transplant. I kept saying in my head “wow, I’ve had a heart transplant, I have someone else’s heart beating in my chest”. I kept thinking of it as ‘the heart’ not ‘my heart’. I didn’t know how to refer to my new heart. Now I call it ‘my new heart’ and the sick one that’s gone I call ‘my other heart’.
On Tuesday morning I was moved up to the less dependent end of CCU and sat in a comfortable chair again all day. The Physios came and took me for another walk and got me doing some other gentle exercises. By this time a lot of the appendages which had been attached to me were off and I just had one drain line out with a small bottle on the end. It was great being free to go to the bathroom again and move around.
I was discharged to the Jim Quick ward on Wednesday. Day 5. I had my own room for a few days which was good. Wound pain had not been an issue since my operation, so I didn’t need many pain killers. I was glad of sleeping tablets because the mixture of all the new drugs I was on made my brain go into overdrive throughout the night if I didn’t take them. I was getting really bad headaches occasionally during the first week, probably due to the medication, so I did take some painkillers for these.
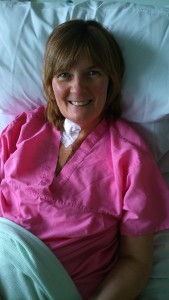
This is me on the Jim Quick ward. I think it was taken on day 6 after my transplant. My husband was really keen to get it onto Facebook to reassure all our family and friends that I was doing so well.
A student Physiotherapist was assigned to me and she came at least once a day, showing me various exercises to do. She was very pleased with my ability at such an early stage after the operation. I felt so much better than I had for years and was raring to go. I walked up and down the stairs in one go without pausing and I was talking as I went. I used to avoid stairs before the operation because I used to get so breathless and exhausted. I would stop every other step to take a big breath. Now I was walking up and down them and chatting at the same time.
I was so elated and amazed at the difference my new heart was making and so grateful. I kept feeling really emotional about the change and the fact that I had someone else’s heart beating so well in my chest. I kept thinking about them. It’s such a strange experience. On the one hand I was elated at having a new start in life but sad and had a sense of guilt about the person who had died. I struggled at first with the thought that someone had died so that I could live, but a friend of mine, who is a retired nurse said to look at it just positively and focus on the fact that this was an amazing gift for me and not to feel guilty that they had died. This helped but I still think a lot about my donor and her family. I’ve since had a letter from her family, replying to my ‘thank you’ letter to them. She was a lovely lady who was always helping others and her family said I couldn’t have received help from a nicer person.
I was continuing to progress well and looking forward to returning home as soon as possible, then a spanner entered the works. My first biopsy showed that my body had produced some new antibodies and they could potentially damage my new heart. Dr. Steve Shaw said it was unusual to develop new antibodies after transplantation. I felt great but had to go through three sessions of plasma exchange. A very cleverly designed machine gradually took my blood out of my body, whizzed it around to extract the plasma then mix new plasma with my blood and return it to my body. This all went well but the day after the third session I was exhausted. This gave new meaning to my understanding of feeling ‘washed out’.
I came home a few days later and continued to make good progress. I attended a second Cardiac Rehab course and the nurses and physios there, who knew me from the previous sessions after my defibrillator was fitted, were amazed and really pleased with the difference in my stamina and strength following my transplant.
Despite being so careful to follow all the post-transplant guidelines about hygiene and food etc; I must have picked up a bug of some sort in August which went straight to my lower left lung and caused really painful pneumonia which needed intravenous antibiotics for 10 days. This really knocked me because I’d been avoiding people with any infections and viruses and been really diligent with the antibacterial gels and cleaners at home.
For years I’d been suffering with a gynae problem which worsened in 2014. In December 2014 I had a total hysterectomy which I couldn’t have had with my other heart due to the risks. I recovered really well from this surgery. My Gynaecologist was impressed with how my new heart performed during surgery. He said it was perfect.
At this stage in my recovery I am attending the Transplant Clinic for biopsies every three months and echocardiograms six monthly. Most of my biopsies have shown no rejection but some have shown mild rejection. My medication often gets changed to balance everything out.
I am gaining strength every day. I walk fast now and do a lot of exercise. I was able to carry on working from home since just after the transplant and am now well enough to go into the office in Liverpool.
Professor Yonan and I at the 1000th transplant celebrations in September 2014
My first Grandchild was born on 25th March 2015 and I am enjoying being a Grandma. Before my heart transplant I couldn’t have held a new born baby standing up without feeling breathless and light headed. Now I am fit and able to help out and look forward to playing with him as he grows up.
This change in my ability would not have been possible if my donor and her family had not made the selfless decision to donate her heart. I will be forever thankful to them for their gift of a new start in life for me.
I encourage everyone to register their consent for organ donation at the Organ Donation Register.